Gastroenterology Appointments 732-597-7333
Gastroenterology Appointments 732-597-7333
Gastroenterology Appointments 732-597-7333
Gastroenterology Appointments 732-597-7333

Barrett’s esophagus is a condition where part of the lining of the esophagus undergoes a change from one cell type (squamous cell) to another (columnar cell). This change is a result of chronic injury to the esophagus from gastroesophageal reflux disease (GERD). Patients with Barrett’s esophagus have an increased risk of developing esophageal cancer. The progression to esophageal cancer typically occurs by some cells in the barrett’s segment becoming more abnormal and atypical, which is called “dysplasia” in medical terms. Patients with this condition usually have their esophagus surveyed every few years to see if they are developing any signs of dysplasia.
Traditionally, the only way to remove the dysplasia before it turned into cancer was by surgery, where the patient would have either a part or the whole esophagus removed. Dr Gorcey is pleased to offer some techniques where both the dysplasia and the barrett’s esophagus can be treated without the need for surgery.
The technique is radio frequency ablation. Through using a device either mounted on a balloon or the tip of the endoscope, heat energy is applied to the barrett’s segment. The procedure is done in the setting of an outpatient upper endoscopy, usually taking between 30 to 60 minutes. More than one treatment may be required to eradicate the dysplasia and barrett’s tissue. The overall complication rate is well under 1%.
In some patients with barrett’s esophagus, there can a raised or depressed area in the esophagus. In this setting, removing the abnormal area using a technique called “endoscopic mucosal resection” can usually be performed. The physician will first attempt to lift the abnormal area or spot by either injecting a water based solution into the tissue or placing a rubber-like band. The physician will then resect it using a snare (wire loop) with cautery (heat energy). The procedure is done in the setting of an outpatient upper endoscopy, usually taking between 30 and 60 minutes. Complications from this procedure include mucosal laceration, esophageal perforation, infection, bleeding, and stricture formation.

Endoscopic view of Barrett's esophagus

The larger the section of Barret's the higher the risk for cancer transformation

We use high definition video endoscopes with high magnification to assess the characteristics of the Barret's tissue. Note the visible gland structures
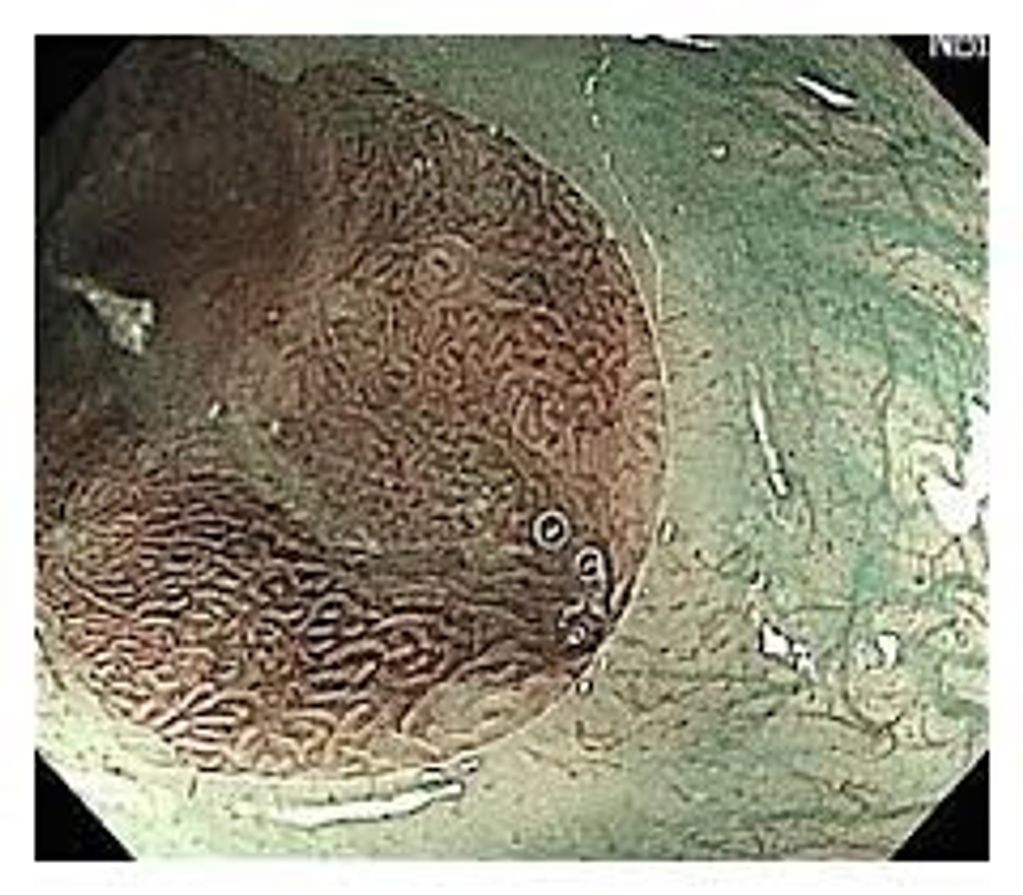
NBI or narrow band imaging is a wasy to better see Barret's changes by changing the wavelength of the endoscope light. Dr Gorcey uses NBI as well as white light during all his endoscopies and colonoscopies (better polyp detection) for a more sensitive exam.

Surveillance endoscopy for Barrett's traditionally utilizes biopsies performed at intervals to monitor for dysplasia and early cancer. Unfortunately, much of the surface area of the Barrett's tissue goes unseen by biopsies. At Monmouth Digestive Health we utilize CDX WATS (Wide Area Tissue Sampling) which involves a special brushing which is the analyzed by 3D computer recognition.
In addition, if Barrett's esophagus is diagnosed, it is sent for another test called Tissue Cypher which can predict the propensity of the tissue to turn to cancer, thereby allowing us to monitor those patients more frequently, or even offer tissue ablation before dysplasia occurs.
Schedule an appointment with Dr Gorcey to discuss treatment options for Barrett's esophagus
We use cookies to analyze website traffic and optimize your website experience. By accepting our use of cookies, your data will be aggregated with all other user data.
Your friendly neighborhood gastroenterologist !! Dr Gorcey
732-597-7333